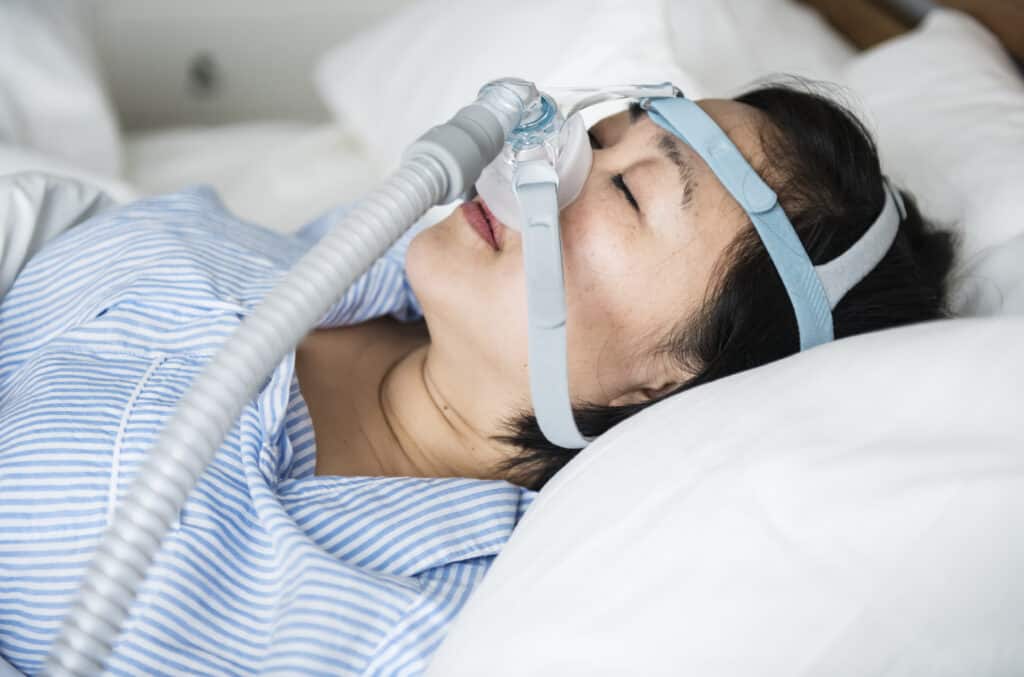
Sleep apnea, a potentially serious sleep disorder, affects many people and can lead to various health concerns if left untreated. One common treatment for obstructive sleep apnea, the most prevalent form of this disorder, is continuous positive airway pressure (CPAP) therapy. This method helps keep your upper airway passages open while you sleep, preventing the interruptions in breathing that characterize sleep apnea.
A CPAP machine delivers appropriate air pressure through a mask worn over your nose or mouth, ensuring stable breathing as you rest. Adjusting to the use of a CPAP machine may seem challenging initially, but with persistence, you can experience significant improvements in your sleep quality and overall health. As you begin your journey with CPAP therapy, stay focused on the potential benefits and remember that any initial discomfort will likely fade with time and consistent use.
Understanding Sleep Apnea
Sleep apnea is a sleep disorder in which your breathing is repeatedly interrupted during sleep, leading to a lack of oxygen and a higher risk of serious health concerns such as high blood pressure, heart disease, stroke, and diabetes.
Types of Sleep Apnea
There are two main types of sleep apnea:
- Obstructive Sleep Apnea (OSA): The most common form of sleep apnea, OSA, occurs when the muscles in the back of your throat fail to keep the airway open, causing a partial or complete blockage.
- Central Sleep Apnea: This type of sleep apnea occurs when your brain fails to send the proper signals to the muscles that control your breathing, disrupting your sleep cycle.
Symptoms
Common symptoms of sleep apnea include:
- Loud snoring
- Pauses in breathing during sleep
- Gasping for air during sleep
- Insomnia or difficulty staying asleep
- Excessive daytime sleepiness
- Morning headaches
- Irritability, mood changes, or depression
- Difficulty concentrating
Causes
The causes of sleep apnea can vary depending on the type:
- Obstructive Sleep Apnea: Factors that contribute to OSA include obesity, enlarged tonsils or adenoids, nasal congestion, a narrow airway, or a receding chin.
- Central Sleep Apnea: The exact cause of central sleep apnea is often unknown, but it can be associated with medical conditions or medications that affect the central nervous system.
Risk Factors
Several factors can increase your risk of developing sleep apnea:
- Obesity: Excess body weight, particularly around the neck, can put pressure on the airway and make it more difficult for the muscles to keep it open.
- Alcohol and sedatives: These substances can relax the muscles in your throat, increasing the likelihood of airway obstruction during sleep.
- Smoking: Smoking can cause inflammation and fluid retention in the airway, leading to a higher risk of sleep apnea.
- Genetics: A family history of sleep apnea may increase your likelihood of developing the disorder.
- Age: Sleep apnea tends to be more common in older adults.
CPAP Therapy Basics
How it Works
CPAP (continuous positive airway pressure) therapy is a popular treatment for sleep apnea disorder characterized by interruptions in your breathing patterns while asleep. A CPAP machine works by using a consistent flow of air pressure to keep your airways open, allowing you to breathe more easily and improving your sleep quality.
Components of the CPAP System
The CPAP system consists of three main parts:
- CPAP machine: This device generates pressurized air to maintain an open airway during sleep.
- Hose: A flexible tube connects the CPAP machine to the mask or nosepiece, delivering the air pressure to your airways.
- Mask or Nosepiece: This is the piece that you wear over your nose and/or mouth, providing a comfortable seal to ensure the pressurized air is effectively delivered.
It’s important to regularly clean and maintain the different components of your CPAP system to ensure its proper function and prolong the life of the equipment.
Different Types of PAP Therapies
In addition to CPAP, there are a few other types of positive airway pressure (PAP) therapies that can be used to treat sleep apnea:
- BiPAP (Bilevel Positive Airway Pressure): This therapy uses two different pressure levels, providing a higher pressure during inhalation and a lower pressure during exhalation. BiPAP can be beneficial if you have difficulty exhaling against the constant pressure of CPAP.
- EPAP (Expiratory Positive Airway Pressure): Unlike CPAP or BiPAP, EPAP uses special adhesive devices that are placed over your nostrils to create positive pressure only during exhalation, helping to keep your airways open.
Your healthcare professional will be able to determine which type of PAP therapy is best suited for your individual needs based on the severity of your sleep apnea and any underlying health issues. Remember that adjusting to CPAP therapy may take some time, but regular usage and proper maintenance can significantly improve your sleep quality and overall health.
Benefits and Drawbacks of CPAP Therapy
Health Benefits
CPAP therapy offers numerous health benefits for those with sleep apnea. By providing constant and steady air pressure, it helps to prevent breathing interruptions during sleep. As a result, you may experience:
- Improved sleep quality
- Reduced snoring
- Decreased daytime fatigue
- Lower risk of heart attack and stroke
Furthermore, CPAP therapy can also help alleviate symptoms of anxiety, headaches, and depression often associated with sleep apnea. Studies have shown that CPAP therapy can lower blood pressure, which may be beneficial even for those who didn’t have high blood pressure prior to treatment.
Side Effects
While CPAP therapy has many advantages, it’s essential to be aware of the potential side effects. Common issues with CPAP include:
- Leaky masks
- Difficulty falling asleep
- Stuffy nose
- Dry mouth
In addition, some users may experience skin irritation or redness due to the mask. To address these side effects, try adjusting your mask for a better fit, using a humidifier with your CPAP machine, or speaking with your healthcare provider about alternative treatments if CPAP is not comfortable.
Remember, finding the right balance for your needs is crucial to maximize the benefits of CPAP therapy while minimizing any potential drawbacks. If you experience persistent side effects or have concerns, consult with your healthcare professional to explore other treatment options or adjustments to your CPAP device.
Selecting and Fitting CPAP Masks
Nasal Mask
A nasal mask covers only your nose, providing continuous positive airway pressure (CPAP) therapy while you sleep. These masks are a popular choice due to their smaller and lightweight design. Adjust the straps and check for any air leaks to ensure proper fit. Periodically clean your mask and replace the cushion or seal to maintain a secure and comfortable fit. Keep in mind potential skin irritation from straps; experiment with strap placement to minimize discomfort.
Full Face Mask
A full face mask covers both your nose and mouth, making it a suitable option for mouth breathers or individuals with nasal congestion. These masks are bulkier but provide an effective seal, especially for those who shift positions frequently during sleep. Adjust the straps around your head and neck to achieve a comfortable fit without unnecessary pressure. As with nasal masks, pay attention to possible skin irritation and clean or replace components regularly to maintain optimal performance.
Nasal Pillows Mask
Nasal pillow masks are minimalistic and least obtrusive, covering only your nostrils. They are a great option if you prefer a lightweight mask or feel claustrophobic with larger masks. Adjust the headgear straps and select the appropriate-sized nasal pillow to ensure a proper fit. Keep in mind that these masks may not be suitable for individuals with high air pressure settings, as the direct pressure directed into the nostrils can be uncomfortable. Regular cleaning and cushion replacement are crucial for maintaining a good seal and minimizing skin irritation.
Fitting and Adjusting Tips
When selecting and fitting your CPAP mask, keep the following tips in mind:
- Take your time: Try on various mask types and sizes to determine the best fit for your facial features and sleep preferences.
- Achieve a secure yet comfortable seal: A properly fitted mask should create an airtight seal without causing discomfort or skin irritation. Adjust the straps as necessary and avoid overtightening.
- Consider your sleep position: Some masks work better for specific sleep positions, such as side or back sleepers. Choose a mask that accommodates your preferred sleeping style.
- Maintenance and care: Regularly clean your mask, replace worn components, and check for leaks to ensure optimal performance and prolong the life of your mask.
By following these guidelines, you can find the right CPAP mask for you and optimize your sleep apnea therapy for a better night’s rest.
Alternative Sleep Apnea Treatments
Lifestyle Changes
Making certain lifestyle changes can greatly improve your sleep apnea symptoms. Some key lifestyle changes for sleep apnea treatment include:
- Losing weight: Excess weight, particularly around the neck, may increase the risk of sleep apnea by constricting your airway. Losing weight can help reduce the severity of your symptoms.
- Avoiding alcohol and sedatives: These substances can relax the muscles in your throat, making it more likely for your airway to close while you sleep.
- Quitting smoking: Smoking harms your overall health and can worsen sleep apnea symptoms by causing inflammation and fluid retention in the airway.
- Regular exercise: Engaging in physical activity can help you lose weight and strengthen your muscles, including those in your throat and tongue.
Oral Appliances
Oral appliances can be an effective non-invasive alternative to CPAP therapy. These devices are custom-made to fit your mouth and work by repositioning your jaw, tongue, or soft palate to keep your airway open during sleep. Examples of oral appliances include mandibular advancement devices (MADs) and tongue-retaining devices. You should consult your dentist or sleep specialist to determine whether an oral appliance is appropriate for your sleep apnea treatment.
Medications and Supplements
While medications and supplements are not typically the first-line treatment for sleep apnea, they may help improve sleep quality and reduce daytime sleepiness. Some medications that can be prescribed for sleep apnea include:
- Modafinil or armodafinil: Stimulant medications that can help reduce excessive daytime sleepiness associated with sleep apnea.
- Antidepressants: Some antidepressants may help improve sleep quality if you have sleep apnea and depression.
However, discussing any medications and supplements with your healthcare provider is important as they may not be suitable for everyone and can cause side effects.
Positional Therapy
If your sleep apnea is primarily caused by a particular sleep position, such as lying on your back, positional therapy may help. This can involve wearing a device or using a specially designed pillow to encourage you to sleep on your side or in another position that may alleviate your sleep apnea symptoms. Consult your healthcare provider to determine whether positional therapy is appropriate for your situation.
Surgical Options
In some cases, surgery may be recommended to treat sleep apnea. Surgical options can include:
- Uvulopalatopharyngoplasty (UPPP): This procedure removes excess soft tissue from the throat to enlarge the airway.
- Jaw repositioning surgery: Also known as maxillomandibular advancement, this surgery moves the upper and lower jaw forward to increase the size of the airway.
- Bariatric surgery: Weight loss surgery can be an option for people with severe obesity who are unable to lose weight through other methods.
Keep in mind surgery carries inherent risks and should only be considered if other treatment options have been exhausted or are unsuitable for your condition. Always consult with your healthcare provider to discuss the best course of action for your sleep apnea treatment.
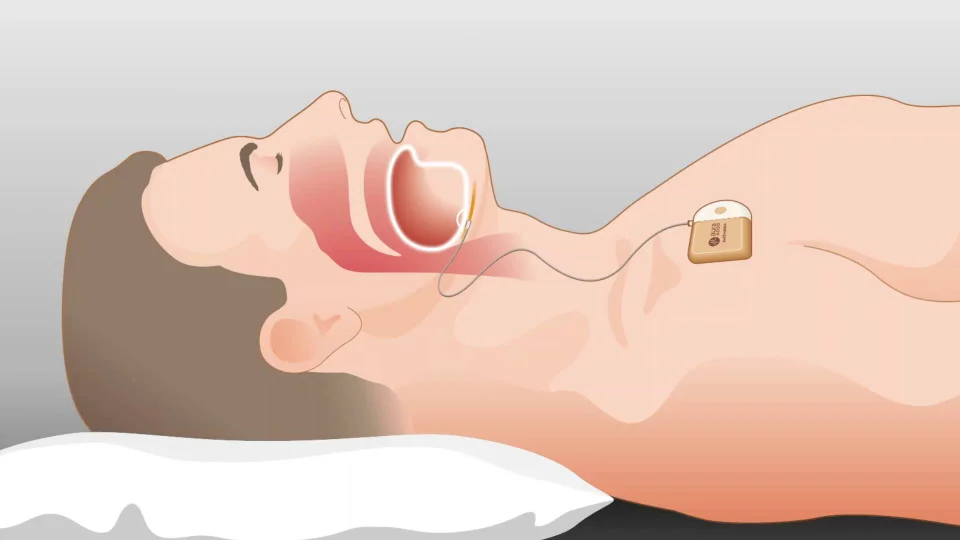
Inspire Implant Technology
Inspire implant technology is an innovative treatment for sleep apnea that uses a small device implanted in the chest to stimulate the airway muscles and keep the airway open during sleep. The device is controlled by a remote that the patient can use to turn it on and off. This treatment has been shown to effectively reduce the severity of sleep apnea and improve patients’ quality of life. However, not all patients are suitable candidates for this treatment, and it requires careful evaluation by a medical professional. Click here to see more information about Inspire implants.
CPAP Therapy and Healthcare Coverage
Insurance Coverage
Medicare may cover a 3-month trial of CPAP therapy (including devices and accessories) if you’ve been diagnosed with obstructive sleep apnea. This coverage extends to CPAP machines, masks, tubing, and other supplies during the trial period. If your sleep apnea symptoms improve during the 12-week trial, Medicare will continue to cover the cost of your equipment. With Original Medicare coverage, you pay 20% of the machine rental plus the cost of supplies such as the CPAP mask and tubing.
Maintenance and Equipment Replacement
Your healthcare provider will guide you on how to maintain your CPAP machine and when to replace parts or the entire device. Some common maintenance activities include:
- Regularly cleaning the mask, tubing, and humidifier chamber
- Inspecting and replacing the air filter as necessary
- Ensuring proper humidity levels to avoid condensation in the tubing
Your healthcare provider or insurance company may also provide guidelines on when to replace parts and equipment, such as:
- Replacing the mask every 3-6 months
- Replacing the tubing every 3 months
- Changing the air filter every 3-6 months or more frequently for certain types
Keep in mind that your specific equipment and insurance coverage may vary for replacements, so always consult your healthcare provider and insurance plan for accurate information.
FDA Approval and Prescription
CPAP machines are regulated by the Food and Drug Administration (FDA) to ensure safety and effectiveness. This means that the devices must meet certain standards before they can be legally sold and used. Obtaining a CPAP machine typically requires a prescription from your healthcare provider, based on your sleep apnea diagnosis and a sleep study to determine the appropriate pressure settings for your device.
In summary, understanding your insurance coverage, proper maintenance, and working closely with your healthcare provider can help you make the most of CPAP therapy for sleep apnea.
Sleep Apnea Diagnosis and Evaluation
Diagnosis Tests and Procedures
During the evaluation process for sleep apnea, the doctor might recommend undergoing overnight monitoring of your breathing and other body functions at a sleep center. Home sleep testing may also be an option for some patients.
One of the common tests to detect sleep apnea is nocturnal polysomnography, which records various aspects of your sleep, such as heart, lung and brain activity, breathing patterns, and blood oxygen levels, among other things. Another test is the split-night sleep study, in which you might be monitored for only part of the night to detect obstructive sleep apnea.
Treatment Plan
If you’re diagnosed with sleep apnea, your doctor will typically recommend a treatment plan tailored to your specific needs. This may include lifestyle changes, such as losing weight, avoiding alcohol, or sleeping in a certain position. In more severe cases, continuous positive airway pressure (CPAP) therapy may be suggested, which involves wearing a mask over your nose and/or mouth that delivers mild air pressure to keep your airways open while you sleep.
Other treatment options may include oral appliances that reposition your jaw and tongue, or in some cases, surgery to correct the underlying cause of the sleep apnea.
Follow-Up
Regular follow-up visits with your doctor are essential to monitor your progress and adjust your treatment plan as necessary. This may involve additional sleep tests to measure the effectiveness of your treatment and to track improvements in your blood oxygen levels. It’s important to discuss any ongoing symptoms with your doctor and to report any difficulties or side effects associated with your treatment.
In summary, sleep apnea diagnosis and evaluation involve a combination of tests and procedures, which guide the creation of a personalized treatment plan that addresses your specific needs. By working closely with your doctor and following their recommendations, you can improve the quality of your sleep and mitigate the risks associated with sleep apnea.
How Sleep Apnea Affects Mental Health
Sleep apnea, particularly obstructive sleep apnea (OSA), can significantly impact your mental health. This section will discuss the connection between sleep apnea and various aspects of mental health, including anxiety, depression, and memory.
When you suffer from sleep apnea, your sleep is frequently disrupted, leading to poor sleep quality. This constant fragmentation of sleep can contribute to the onset or exacerbation of anxiety and depression. A lack of quality sleep can leave you feeling irritable, fatigued, and more susceptible to stress, making it difficult to cope with daily challenges.
In addition to affecting your mood, sleep apnea can also impact your cognitive abilities. Persistent sleep disturbances can hinder your ability to concentrate, process information, and maintain focus. Over time, this can lead to memory problems and difficulty retaining new information.
Furthermore, sleep apnea is associated with decreased blood oxygen levels during sleep, as indicated in this Cleveland Clinic article. When your brain is deprived of oxygen, it struggles to perform essential tasks, potentially exacerbating existing mental health issues or contributing to the development of new ones.
To summarize, sleep apnea can adversely affect your mental health in several ways, including:
- Increasing anxiety and depression
- Impairing memory and cognitive function
- Reducing overall sleep quality
Addressing sleep apnea through treatment methods like CPAP therapy can help alleviate these mental health concerns and improve your overall well-being.
FAQs
What is CPAP therapy for sleep apnea?
Continuous positive airway pressure (CPAP) therapy is a common treatment for sleep apnea that involves using a machine to deliver a continuous flow of air pressure to keep the airway open during sleep.
How does CPAP therapy work?
The CPAP machine delivers air pressure through a mask that the patient wears over their nose, mouth, or both. This air pressure helps to keep the airway open, preventing apnea episodes (breathing pauses) that occur during sleep.
What are the benefits of CPAP therapy?
CPAP therapy can help to reduce the severity of sleep apnea symptoms, improve sleep quality, and decrease the risk of complications associated with untreated sleep apnea, such as high blood pressure and heart disease.
Are there any side effects of CPAP therapy?
Some patients may experience side effects such as nasal congestion, dry mouth, or skin irritation from wearing the mask. These can often be managed with adjustments to the mask or machine settings.
How do I get started with CPAP therapy?
A medical professional will evaluate your symptoms and recommend the appropriate treatment, which may include CPAP therapy. You will then need to obtain a CPAP machine and mask, which can be obtained through a medical equipment supplier. A healthcare provider will also help you with machine settings and mask fitting.